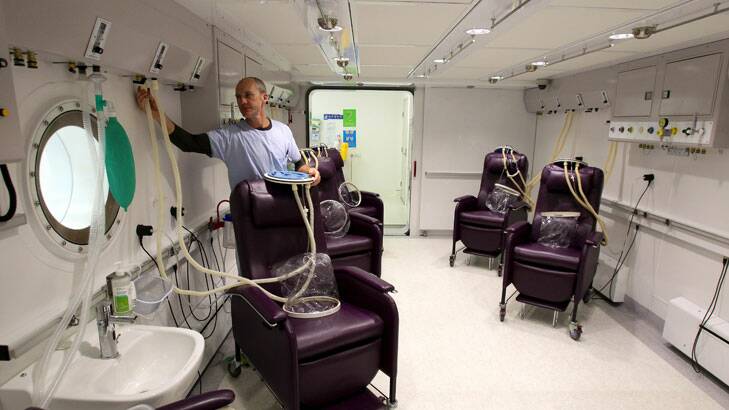

When Chris Francis went to Sydney's Prince of Wales Hospital's hyperbaric unit in January, she was in a world of pain and could barely walk.
A year earlier, Francis, of Newport, had undergone radiotherapy after having a small skin cancer removed from her shin. The treatment destroyed the cancer cells, but also the surrounding tissue.
"I had a great big hole in my leg," Francis says. She ended up bedridden for three months. "Just to stand up and clean my teeth and go back to bed was agony."
She was eventually referred to the PoW unit at Randwick. After six weeks of daily therapy and regular wound care, her ulcer was "looking really good"; three months further on, it has all but disappeared.
While many people may know of hyperbaric oxygen therapy as a treatment for "the bends" (decompression sickness in divers), Francis is more typical of the majority of patients undergoing hyperbaric therapy at hospital-based hyperbaric units across Australia.
About half of the patients at PoW are being treated for damage to bone or soft tissue incurred during radiation therapy. Almost a third are there because of non-healing ulcers, chiefly diabetic ulcers. Divers are the next biggest group, followed by small numbers of patients with problems such as necrotising infections, carbon monoxide poisoning and Crohn's disease.
Patients sit or lie in a sealed chamber and breathe 100 per cent oxygen – compared with the 21 per cent found in normal air – at depths equivalent to 10-20 metres under water. While the lungs are saturated with oxygen, the increased atmospheric pressure drives the gas into the body's tissues much more rapidly than under normal atmospheric conditions. This can allow tissue that has not been getting the blood and oxygen it needs to heal to begin that process.
For some people who have suffered tissue damage during eradication of cancers in the pelvic area, for example, "their problem is just unremitting", says associate professor Mike Bennett, a doctor at the PoW unit and president of the South Pacific Underwater Medicine Society.
"And the only solution until recently [has been] very major, radical surgery – removing the bowel, removing the bladder, having all sorts of bags and tubes permanently attached to your tummy.
"Hyperbaric has turned around some of these people's lives. It allows the tissue to repair itself, so the bowel or the bladder or whatever's damaged, over a period of weeks to months, slowly repairs itself and normal function, or close to normal function, is restored."
Yet how the therapy works remains poorly understood. "It's almost certain there are lots of things happening at once [in the body]," Bennett says. "One thing we do know is if you just have more hyperbaric – that is, you spend twice as long in the chamber – it doesn't work any better; often it works less well."
Treatment regimes differ with different disorders, but in most cases the therapy involves 1-2 hours a day in a chamber for 20-30 days.
Although it has been around for more than 50 years, hyperbaric therapy's uptake across countries and states varies – as does GPs' and specialists' knowledge and acceptance of the therapy.
"There's lots of things that people give hyperbaric for where there's no prospect of improvement," Bennett says.
He divides potential patients into three groups: "Those we're pretty confident we can help, and the evidence is there and the figures are on their side", such as people with diabetic ulcers or radiation damage; disorders for which researchers and practitioners are confident [it] doesn't work, such as cerebral palsy and autism; and "a whole lot of things in the middle where no one knows. There may be rational reasons to think 'hyperbaric might be good for that', but the evidence isn't there."
Part of the PoW unit's work is treating some of those grey-area cases and gathering more data about whether hyperbaric therapy may be of benefit – cases such as sudden hearing loss, Crohn's disease and non-diabetic ulcers (Medicare covers the therapy as a treatment for diabetes-related ulcers but not other non-healing wounds).
Internationally, an emerging area of interest is hyperbaric therapy as a way of preventing a harmful inflammatory reaction – known as a reperfusion injury – that occurs in some heart-attack and organ-transplant cases.
Most doctors involved in hyperbaric medicine are anaesthetists, while nursing staff usually have an emergency-care or ICU background as well as hyperbaric qualifications.
"It's a totally different world in [the chamber] . . . once the doors are shut, there's no getting out or getting in in a real hurry," says Brian Reed, a nurse at PoW.
Claustrophobia can be a problem in the chamber; some patients experience crackling in the ears, temporary changes in vision or – very occasionally – a seizure.
Chris Francis was relieved when her treatment was over but says it was worth it. "Just to be able to walk outside [again] and hang the washing on the line, do housework – I never thought I'd enjoy that, but I'm just enjoying all that. Being free."
Medicare funds hyperbaric therapy for these conditions:
Radiation injury to soft tissue or bone.
Diabetes-related non-healing wounds.
Gas gangrene.
Necrotising soft-tissue infections.
Decompression illness.

